I’ve contemplated how to write this birth story for a very very long time. I’ve never shared the births of any of our children. I have always reserved it as a journey for just our family – specifically me and my husband (Joseph). No matter how it goes, every birth is so deeply personal. But as I lay in the hospital bed after the birth of our third sweet babe, I felt compelled to share the experience. I don’t know why, and I don’t know quite how. But I’m going to do my best.
A word of warning – it’s a bit of a long one.
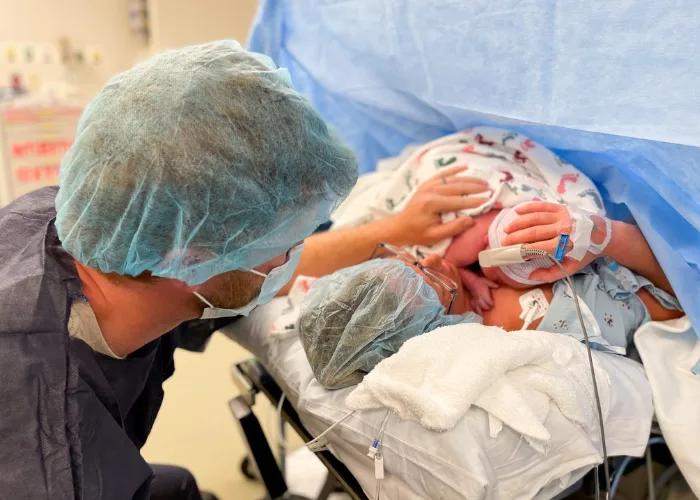
Let me first preface this by saying, I am eternally grateful for our healthy baby boy. I do not take it for granted, and I am so thankful for the doctors that brought him safely into this world. Life is always a gift. But that does not negate the trauma I had to work through afterwards. It does not negate the fact that his birth was very hard on me. It took me a long time to realize that.
I can be both grateful and hurt. That’s ok.
If you’ve experienced a traumatic birth, you can be both grateful and hurt. That’s ok.
I’ve hesitated to write this because I don’t want it to come across as an “oh, poor me.” I truly just want to share the story in case it can help anyone else who’s experienced a traumatic birth. If it helps just one person feel seen and heard and understood, then it’s worth it. You are not alone.
It’s been about a year and a half since he was born. When I first started thinking about how to write this story, I was so hurt and angry at the whole event. I was angry at the doctors. I was angry at Joseph. I was angry at myself for not standing up for myself more firmly. I felt broken – physically, mentally, emotionally. It was a long road to work through it all.
For a long time, it felt weird to say the birth was traumatic when I have a beautiful, healthy baby at the end of the day, and so many people are suffering such greater trials. It seemed so small and insignificant. But, if there’s anything I’ve learned through processing the trauma, it’s that you have to accept that it was traumatic. That it wasn’t what you wanted. That it did hurt. It doesn’t have to be the exact same brokenness or the exact same trial. We all have different crosses to bear.
Once I was able to say that to myself, I started to open up to more people about the experience, and, to my surprise, people opened up in return. Infertility, miscarriage, birth trauma – I’ve had friends and family touched by all of it. And no one ever mentioned it until I opened up my brokenness to them. We’re all broken. Being broken opens our hearts. It can be very beautiful. It invites others to share their brokenness and, suddenly, we realize that none of us is alone. And, in accepting and processing our trauma, we can be there better for other people who are walking through their trials. It’s how we learn to love – to be kind, to be open minded, to empathize with each other.
This is the birth story of Arlo Joseph.
Leading Up
Let me start with some of the surrounding events. Without the events in the months and weeks leading up to his birth, I don’t think it would have hit me quite the same and, quite honestly, changed my life forever. I mean, new babies always change your life forever. But this was different. It was one of those pivotal moments that you look back on and say, “yeah, that changed the trajectory of my life.”
After waiting for 3 years for an opportunity to move back to my hometown in Montana, we finally got the go-ahead from Joseph’s company that he could work remotely. I was a few months pregnant at the time, but everything seemed to be going smoothly (unlike my second pregnancy). We figured we’d have just enough time to move, find a house, and switch doctors before baby arrived. Though the timing could have been better, it was our best shot at ever making the move, and we felt we couldn’t pass it up. The events that lined up for us to be able to move at all were nothing short of a miracle. You know those times where everything seems to line up perfectly, pointing you in the correct direction? One of those times.
We sold our house within a week of listing and started searching for a new one. Once our Minnesota house closed, we made the long trek to Montana and moved into my dad’s for a few weeks. We closed on our second home on our 5th wedding anniversary (strange coincidence), and moved in a couple weeks later. I was well into the third trimester.
Meeting my New Doctor
During this time, I met my new OB doctor at 34 weeks pregnant. She came highly recommended and was very well-known around town. The first appointment went well – discussed my history and made sure baby looked comfy cozy in there. All good. I have an interesting pregnancy and birth history, so I was nervous to switch doctors but felt comfortable in her care.
With our first babe, I hemorrhaged pretty severely during/post delivery. I have a blood disorder that makes me slightly anemic at all times, so there’s much less room for error with blood loss. I stayed just barely above the line for blood transfusions after his delivery, but, because of all the blood loss, struggled pretty hard with recovery for the first couple weeks. Our second babe ended up being a high risk pregnancy – a case of severe hemorrhage early in the pregnancy (around 8 weeks and they told me there was about a 50% chance I’d lose her at some point), then severe IUGR (intrauterine growth restriction), significant restriction in the blood flow through the umbilical cord, and ended with induction at 37 weeks and a stay in the NICU. I also hemorrhaged after/during her delivery and then had to have a D&C for retained placenta a few weeks later.
So, given my history, they were watching me more closely with this third one and tracking his growth every few weeks. My new doctor scheduled an ultrasound to check his growth, as recommended by my previous doctor, and I went it for it the next day following that 34 week appointment. To everyone’s surprise, baby was breech. Footling breech, no less. Which explained why it felt like he was jumping on things he shouldn’t be jumping on, and I couldn’t breathe (hello large head in my ribcage and lungs). It had been my most uncomfortable pregnancy, physically, and had gotten significantly worse since my previous appointment back in Minnesota a few weeks earlier. It all made a lot more sense once we figured out how he was positioned and that he was getting quite a bit bigger now.
The ultrasound tech let me know that most babies flip over by 36 weeks and everything would probably be just fine. She said the doctor would confirm the position again at my next appointment, but hopefully he’d flip by then.
36 Weeks
My next appointment was at 36 weeks. I went in, and she confirmed that baby was indeed still footling breech. I asked what that meant for birth and she candidly replied, “C-section, unfortunately. Look up spinning babies for methods to try to help flip baby and next time we can discuss a version if he’s still breech” as she walked out of the room to move on to the next patient. That was it.
Joseph wasn’t with me, so I just sat there alone, shocked that things had taken such a quick turn. I had never even considered I’d end up in a c-section, let alone with a brand new doctor in a hospital I don’t really trust. I was particularly afraid of c-sections, given my anemia and history of post-delivery hemorrhage, since you usually lose about twice the amount of blood as during a normal delivery, assuming you don’t also hemorrhage during the surgery. The thought of losing twice the amount of blood just to start with (since it’s a major surgery) and then potentially hemorrhaging in addition to that, and already being slightly anemic in my “normal” state, had me pretty terrified.
Now, yes, I know doctors are very busy and over-scheduled. One of my sisters is a doctor. I understand the stress and workload they’re under, and I know they’re doing their best. But I did not feel well taken care of at that appointment. I was just another patient to rotate through as fast as possible, without regard to my fears or concerns about a c section. There was no discussion, no options, and no concern for me as the mother – just a “yep, c section.” I felt incredibly unseen and unheard.
So I did all the research I could possibly do, tried all the spinning babies methods to flip a breech baby, starting seeing a chiropractor who knew the Webster technique, and spent so much time on my hands and knees that they were pretty much raw (on all fours is a great position for getting baby into good positioning or helping a breech baby flip). With most of the methods, I could get him to move around quite a bit and squirm and readjust, but never felt a big rotation.
37 Weeks
After a week of trying to get him to flip, I was ready for my doctor to check his position at the 37 week appointment and discuss the option of a version if he was still breech (which I figured he was since I hadn’t felt any big rotations in the past week). But a couple hours before the appointment, I got a call from the doctor’s office that she had to cancel my appointment because the doctor was headed over to the hospital to do a c-section for another patient. Totally understandable. But the office told me they didn’t have any other appointments available for the week and couldn’t reschedule. They told me that no provider in the office had any openings, so I could just wait until the following week for my 38 week appointment. Again, I understand that they were over-booked and under-staffed and everyone was doing their best. But having the 37 week appointment cancelled when my baby was breech was a little crushing and unnerving. I mean – I was a ticking time bomb at that point. And my doctor had told me she recommended we schedule a version for that week if he was still breech, before he grew much more.
I was not in a good headspace at this point. I was pretty certain he was still breech and was terrified of ending up in a c-section. We started discussing the option of traveling back to Minnesota so I could at least be with my doctor who I knew and trusted, in a hospital I had delivered at before. Whether it ended up in a c-section or not, at least I knew the doctor and would trust the decision. A few of our close friends were getting married that weekend back in Minnesota. We had originally planned that Joseph would just travel back quickly for the weekend since I was so far along. But, after the 37 week appointment cancellation, we decided we’d all go and see if I could get in with my original doctor, or at least see a doctor in that practice (I knew quite a few of them from my second pregnancy since I had to go in so often). I called them to get on the cancellation list (in case anything opened up sooner) and made an appointment for Wednesday, which was still 1 day earlier than my new doctor was going to be able to fit me in.
Joseph and I decided we’d feel things out for the weekend and wait for some sort of intuition or something to stay in Minnesota or head back to Montana. That probably sounds crazy. I know. But, honestly, I just felt completely alone at this point. No doctor would see me. We had just moved across the country. We were homesick. I was looking for anything familiar that might offer some peace in the unknown I was facing.
Nothing.
We went back and forth on what to do. Talked about logistics if I had a c-section in Minnesota, when we’d be able to get back to our new house, and what it would that look like with an infant and two toddlers staying at my husband’s parents’ house.
Over that weekend, I had some serious prodromal labor – enough to keep me up at night. Then it would stop every morning once the kids were up and the day got going. Looking back, I think my body knew he was in bad position and was trying to get him moved around. But he was pretty crowded in there at this point and there wasn’t much space for movement. I tried every. single. spinning babies technique I could, especially during the prodromal contractions. I was really trying to work with my body and baby to get him flipped over.
Fast-forward to Tuesday – I got a call from my new doctor in Montana that she wanted to do one more ultrasound to confirm he was still breech before we discussed a version at the next appointment. The ultrasound would have to be Wednesday afternoon. So for a few hours I had an appointment at 9am on Wednesday in Minnesota and an appointment at 1pm on Wednesday in Montana. Tuesday evening we finally made the decision to head for Montana, with the reasoning that, despite the familiarity and trust in my doctor in Minnesota, we needed to be in our own house when the new baby arrived, however that was going to happen. Within a few hours, we were packed and driving overnight to make it back in time for the ultrasound the following afternoon (its about a 17 hour drive).
38 Weeks
I went in for the ultrasound, and they again confirmed he was still footling breech. The next day, I went in for the appointment with my doctor. Joseph was with me this time and we discussed the pros and cons of a version. We decided to give it a try and made the appointment for the following Tuesday. That put me at 38 weeks 5 days – over a week later than she originally told me she would want to do a version.
At the same time, we made an appointment for a scheduled c-section on Thursday in the event the version was unsuccessful. Now, I’m not a super “crunchy” mom (and even less so back when this was all happening), but I’ve always approached things with a view of “let’s leave things as natural as possible and only intervene when necessary.” The last thing I wanted was to schedule a c-section. But I knew the risks associated with footling breech and didn’t really feel like I had a choice. Regardless, I was very uneasy about the scheduled c-section and figured I’d just cross that bridge if we got to it, hoping the version would be successful and it wouldn’t be an issue.
External Cephalic Version
What is a version? It’s a procedure to try to flip a breech baby manually. But they prep you just the same as if you were getting ready for a scheduled c-section. I think just in case it ends up in a c-section since it is very stressful for both mom and baby, though I felt like they were prepping me for a failed version before we even started. But alas, that’s how it goes I guess.
On Monday, I got all the pre-surgery calls, had my blood drawn in case of emergency, went through the check-in procedures, quit eating the night before (in case of an emergency c-section), and my mom picked the kids up so we could go in for the version the next morning.
I had one last chiropractor appointment to see if maybe he’d move on his own. As I was walking out, a sweet old man stopped me in the hallway to ask when I was due. I broke down in tears and told him it was supposed to be July 1, but baby’s breech so possibly the next morning. He was so so kind and gentle. I was just a random lady in the hallway at the chiropractor, completely broken down, and he told me the story of his daughter’s second baby. They had tried a version to flip baby but ended up in a c-section. Turns out, that was the best thing that could have happened because baby was all wrapped up in his umbilical cord – under his armpit and up around his neck. He told me she went on to have a beautiful VBAC a couple years later with twins, no less. He gave me a sweet hug and said “I’ll be praying for you both.”
It was the kindest meeting and, truthfully, gave me the courage to walk into the hospital that next morning. I have no idea who that man was, but I will always remember his kindness – a guardian angel letting me know everything was going to be ok. I felt like I was facing this great unknown, and he gave me some calm to face it. It’s bringing tears to my eyes as I write.
The rest of the evening was kind of surreal. We were supposed to go home after the version, whether it was successful or not, unless there was an emergency. And the scheduled c-section was on Thursday if it didn’t work.
Do we pack hospital bags? Are we going to meet our third precious babe tomorrow? Is everyone going to be ok? I packed a bag, just in case, but for some reason Joseph didn’t. I don’t remember why I did and he didn’t? But that’s what happened. We headed to bed early and planned to get up around 5am to head to the hospital (they have you come in at surgery time).
Ok – I’m going to be very open about everything that happened. It’s all TMI, but this is a birth story after all.
Tuesday, June 22. Midnight ish? I woke up feeling very uncomfortable and having pretty regular contractions. The only thing that helped a little was sitting on the toilet or getting on my hands and knees on the floor. Now, I’d been through two births before this, so I knew exactly what was going on – if I’m on the toilet or hands and knees, it’s because I’m starting labor. It’s been the exact same with every baby. Then I lost the mucus plug. Yep. Things were definitely starting to move.
I moved back to the floor and remember being there on hands and knees, trying to get into any kind of position that might help baby flip during the contractions, and thinking “This can’t be happening. This can’t actually be happening. He’s not facing the right direction and we’re supposed to flip him in the morning. He can’t be trying to make his way yet.” For me (with all 3 kids), labor usually starts slow and is just fairly uncomfortable for a while, but nothing crazy. But I knew it was the start.
I went back and forth on whether to wake Joseph. I briefly considered just skipping the appointment for the version and heading in once I was really in active labor. Then I thought maybe it was just the stress, and I should try to sleep some more. But that wasn’t happening at that point. So I just worked through the contractions and tried all the different positions for moving a baby around in early labor. Once 5 am rolled around Joseph got up and we got ready to go. As we were walking out the door, I told him I thought I may be in early labor and had been up most the night with contractions about 5 minutes apart and had lost the mucus plug.
Neither of us knew if they could even do a version when you’re in labor, but we headed to the hospital to find out.
Hospital
We made it to the hospital and got all checked in. I remember standing there thinking “why is this lady taking so long with all the paperwork? Doesn’t she know I’m in labor?” Of course she didn’t because all the paperwork said I was there for a version. Well, it actually said I was there for a scheduled c-section and I had to correct her that I was there for a version – another time I did not feel very well cared for. How do you mess up the information on what procedure someone is coming in for? But, anyways, I didn’t say anything to her about possibly being in labor. Looking back on it now though, I guess I was still having some contractions and was pretty uncomfortable standing there.
They took us up to the room, and I told the doctor and nurses I thought I was in early labor. They hooked me up to some monitors and confirmed that I was, indeed, having regular contractions and in labor. I remember the nurse looked at me during one of the contractions and asked, “can you feel that?” I thought to myself, “Lady, of course I can feel that. It’s been hours of this and this is my third child. I know what’s going on. It doesn’t feel great.” But I just said, “Yes, I can feel that.”
She said, “Let’s just give it a couple more contractions before we start the version. We had another mom in here last week for a version, but then she had one contraction and boom – baby flipped right over.” I know she had good intentions, but it was another time I felt unseen and unheard. I had had prodromal labor for weeks and early labor contractions for hours and baby hadn’t flipped. I remember my heart just dropped when she said that. No. He wasn’t going to move. If he hadn’t moved yet, he wasn’t moving on his own.
Fast forward a few contractions later and he was still very breech. So they informed me that they would give me a shot before the version to relax my uterus and that would stop the contractions for a few minutes while they tried to flip baby.
The Version
They laid the bed all the way down and tilted it slightly upside down (ever so slightly – you can just tell that you’re not totally flat). The goal is to get baby up out of the pelvis so they have some room to move him. The doctor looked at me and said “I’m sorry. This is going to be a bit uncomfortable but try to relax through it as best as you can.”
I have a pretty decent pain tolerance. My first birth was unmedicated, with Pitocin. My second birth was induced, Pitocin again, and I got an epidural just 10 minutes before she was in my arms – which is a whole different story, but I went through most of labor without anything and could still feel most of the transition and delivery. I would describe that experience as the epidural took the “sharpness” of the pain away, but I still definitely felt a lot. Regardless, I’ve been through the whole thing with no pain relief before, so I’m aware of what that feels like.
When they started the version, it was incredibly painful. I’ve since learned that many hospitals offer epidurals during a version (or some kind of pain relief) because they’re so painful, especially that far along with a baby that size. However, this hospital does not offer pain relief during the procedure, just in case you have to go to an emergency c-section and they need to give you a spinal block. If you have an epidural, they cannot give you the spinal and just have to knock you all the way out under general anesthesia. I’ve also heard some women say a version is not painful at all, just a little uncomfortable. I’m sure it depends on mom’s size, baby’s size, baby’s position, and the method of the doctors. This was not just a little uncomfortable. The version I had was very painful. It was not a gentle flip by one doctor, like I had watched in the videos online.
There were two doctors – one on each side of me to get the best grip on baby – and a nurse with the ultrasound to monitor baby and make sure he was handling it ok. The two doctors leaned all their body weight down into my belly to grip baby and start to try to move him, while the nurse tracked his head on the monitor. Yes, there were three people on top of me. I tried to relax as much as possible as tears ran down my cheeks. It hurt, and I was so worried for our little babe. I had no idea how brutal the version was going to be for either of us. I did not feel like they prepared me for it at all. It may have been uncomfortable a week earlier when baby was a bit smaller, but it was incredibly painful with a full-grown babe as stuck as he was.
Later, Joseph told me that he could see the whole shape of Arlo as they were trying to move him – that’s how hard they had to push to get a grip. They tried a few different grips and switched directions a couple times to see if anything would work, but his butt and feet were really lodged in my pelvis. They continued for about 5 minutes, and then gave us a rest.
The doctor asked me if it would be ok if she tried an internal version while the other doctor continued to try to flip his head with the external version. And, yes, that’s exactly what it sounds like. It was incredibly “uncomfortable”. So she did an internal version to try to push him up out of my pelvis while the other doctor gripped his head and rotated downward from the outside of my belly.
Then I felt a warm gush, and I knew we were done. My water broke.
My doctor looked at me from the foot of the bed, and I, rhetorically, asked her what that meant. She told me they could try one more time with the internal and external version, but baby wouldn’t have much, if any, fluid to float in and the risk of preeclampsia was much greater. She informed me I was already dilated to 4-5 cm and 100% effaced and recommended we move to a c-section. This hospital does not support breech birth. It brought me some consolation to know that he was coming that day, whether by c-section or not, but it was still very much not the outcome I had hoped for.
She asked if I wanted to walk to the operating room. I told her it felt like his foot was going to fall out if I stood up. She confirmed his foot was right on my cervix and that it was almost dilated enough that a foot might slip through – things you never think of when a baby is head down, but if they’re footling breech, one of the dangers is that a foot (or feet) can come through the cervix before the rest of baby will fit. It increases the risk of preeclampsia drastically since the umbilical cord can fall through so easily with the feet. I’ve read stories of women who’ve delivered a footling breech vaginally. But, at the end of the day, it wasn’t worth the risk to me. I knew it was time to make the decision I had so desperately wanted to avoid. So, as tears streamed down my face, I said yes let’s go.
I remembered the kind old man the day before who said he’d pray for me that morning, as well as a friend who had told me was going to offer his morning Mass for me – which happened to be almost the same time that this was all happening. A few months prior, my mother in law had told me the story of one of her closest friends who had a scheduled c-section and that it was the most peaceful, beautiful delivery she’d ever had (after 5(?) vaginal births and one prior c-section). I held all of them in my heart as they wheeled me toward the O.R. They will probably never know, but they are the only reason I didn’t completely break down in that moment. After waiting and contemplating and fighting this event that I had known was coming for weeks, they gave me the strength to make the decision that had to be made that morning, no matter how badly I didn’t want to.
If you’ve ever had a c-section, you know that your husband or support person is not allowed to be with you until the spinal block is in and everything is ready to go. So they wheeled me, alone, down the hall and into the O.R. while Joseph got scrubs on and waited in the other room.
The Delivery
Though I had not felt well-cared for leading up to the c-section, I am very fortunate that the anesthesiologist and nurses in the O.R. were very kind. I know that is not everyone’s experience who ends up in a caesarean, and I’m very thankful.
As I sat on the table and they put the spinal block in, a wonderful nurse held my arms and steadied me. She told me I was handling things well, though she knew this was not what I wanted and she knew it was very overwhelming. Just feeling seen in that moment made all the difference.
The anesthesiologist talked me through everything as it was happening and held the puke pan for me as the spinal did its work (I guess it’s fairly common for a spinal block to make you very nauseous and/or sick). He was so kind and let me know that things were going smoothly, I’d start to lose feeling soon, and mine and baby’s vitals were all still looking good.
They laid me out on the table as everything started to go numb from my ribcage down. They lay you flat on your back and spread your arms out to the side when they do a c-section, so I just laid there with my head turned as best as possible into the small puke pan by my head. The anesthesiologist gave me another medicine to curb the nausea, which calmed it down in just a few minutes, and then Joseph was finally allowed in the room.
Joseph later told me that he thought something had happened or that they had forgotten about him because he waited in the room for so long before anyone came to get him. I can’t imagine what that must have felt like. But once he was there, they confirmed that I was sufficiently numb, and began the surgery. I learned later when they “checked” if I was sufficiently numb, they had already started cutting and just asked if I could feel anything. Thank goodness, I could not. I have a friend who was in such an emergency situation that they had to start cutting before she was numb. I can. not. imagine.
As the doctors cut me 7 layers deep, wide open, they chatted like normal – just another day at the office. I’m still not sure what I think of that whole thing. Maybe it was calming to hear normal conversation? But it was also a little weird considering the situation and how absolutely terrified and distraught I was. I’m not sure. I don’t know if silence would have been any better though.
It was a strange experience. No pain during the operation – just a lot of tugging and pulling, which made me a little woozy, in addition to the spinal block that had already made me sick.
And then they held him up and over the curtain – our beautiful 7lb 1oz baby boy. He was quiet. They rushed him over to the nurses station, where they worked quickly to clear his lungs and get him breathing. They had a NICU unit in there, just in case, as well as the pediatrician and a few nurses. He finally cried. His neck was very kinked to the right and the left side of his head was all pressed down flat where he had been stuck in my ribs, but he was perfect. They wrapped him up, brought him over, and I got to hold him as they stitched me back together.
I did not hemorrhage any more than normal during the surgery. I lost about double the amount of blood as during a typical vaginal birth, which is pretty standard for a caesarean. It was about the same amount of blood I had lost with the hemorrhaging during the birth of our first babe. Due to my blood disorder, I was close to the limit for a blood transfusion, but they just kept a close eye on me over the next few days to make sure I recovered. The blood loss definitely made the first few weeks of recovery very slow. But, relatively speaking, it went smoothly.

Welcome to the world, Arlo Joseph.
They had started the version around 8:30 and he was in my arms by 9:30 via c-section.
We moved to a recovery room. Even though I had had a c-section, they still have to do the thing where they push down on the top of your uterus (fundal massage) to make sure it was cramping back down correctly and fast enough. Who knew. I thought it was bad when they do that after a vaginal birth. It really doesn’t feel good after a c-section. Every 15 minutes. Then every half hour. Then every hour for a couple hours. Why.
A few hours later, they had me stand up and try to walk and go to the bathroom.
I had absolutely no idea how intense a c-section recovery is. No one prepared me for that. The doctor talked about the c-section like it was no big deal. It is, in fact, a big deal. Having had both experiences, I would rather give birth vaginally 1000 times than ever have another c-section.
My doctor later informed me that she found meconium in my uterus during the c-section. When my water broke during the version, it was all clear (which usually means no meconium). So Arlo had definitely gotten stressed out at some point after the version, before the caesarean. The weird thing is, I knew when my water broke that it was time to go to a c-section. I just had a gut feeling not to try to flip him anymore. I’m so glad I followed that intuition – thank God for the weird mom-baby connection. Where we live, there isn’t a NICU unit in our hospital that could have handled it if he had aspirated the meconium. There’s a basic NICU unit, but he would’ve had to have been life-flighted to the nearest full NICU.
God Hints
I feel like we’re closest with God in the events around both the end of life and the arrival of new life. In both death and birth, we’re so close to the source of existence. It’s almost as if the veil is thinned just a bit. Looking back, there were a lot of moments in the few weeks leading up to Arlo’s birth that prepped me for what was going to happen – the man at the chiropractor, my mother-in-law’s friend, and my friend – to name a few. I just had a weird feeling that I was headed for the c-section, no matter what, and that it was what had to happen. That’s not to say I was happy about it at all. It was painful in every way. It felt like I surrendered my body, my mind, my pride, my self.
After going into labor the night before, the external version, the internal version, and then a c-section, I felt like I had been hit by a truck. And I felt like no one understood. I was alone again. I know that’s not true. And, looking back now, if I had to do it all again, given the circumstances, I would still decide to go into the c-section. But, at the time, I felt like I had been pushed around by the doctors who didn’t care enough to see my at my appointments, brutalized by the version that no one really prepared me for, and literally ripped apart by a c-section that no one really prepared me for either. Then sent home to take care of an infant when I could barely stand up.
I also think a lot of the trauma came from my desire to have a normal, uncomplicated, natural (unmedicated) birth for our third child after a rather complicated and scary pregnancy and delivery of our second babe. I wanted to prove to myself that I wasn’t broken.
It was not the natural birth I had longed for. I did not “prove” to myself that I wasn’t broken. Not at all.
Then, I had a very long, tough recovery. Did you know that, under normal circumstances, it takes about two weeks for your body to replenish blood volume after a significant loss of blood? I’m not sure how long it takes after pregnancy and a c-section when your whole system is also trying to repair the cut through your abdomen as well. All I know is I had a tough recovery after blood loss from the hemorrhage with our first and I had a very tough recovery after the blood loss from the c-section (both nearly the same blood volume). It took weeks before I could stand up for more than 5 minutes at a time without getting really dizzy, in addition to the normal difficult recovery from a caesarean. Again – no one prepared me for that. It was nothing like I had ever experienced with my other two births.
You Should Be Thankful
When I first tried to tell my story, I had a few people tell me “Yeah, but you have a beautiful, healthy baby boy. You should be thankful to be able to have kids and that you’re both healthy. It’s a blessing.”
Yes, it is a blessing, and, again, I was (and am) so SO thankful. But it has taken me a year and a half to work through everything that happened.
At first, I felt so guilty for feeling bad about the birth. I felt guilty for feeling like a failure. I felt guilty for not just being over-the-moon happy that both me and Arlo made it through everything and were both healthy. I felt guilty for feeling guilty.
So. Much. Guilt.
“It doesn’t matter what happened to me because I have a healthy baby and I should be thankful, not unhappy with how it happened.” That’s what I kept telling myself.
I was telling one of my friends the story and she stopped me and said, “It’s ok to say it was traumatic. It’s ok to mourn the birth. That’s ok. That’s normal.” It was the first time I felt seen and heard and was given permission to be hurt by the experience. It was the beginning of figuring out how to heal from it.
Processing
I started reading and listening to countless birth stories from other women. It was so important in my healing process and much of the reason I wanted to write my own story down. I found The VBAC Link Podcast to be incredibly helpful. They bring women onto the podcast and simply let them tell their stories. A huge turning point for me was simply realizing that I was not alone.
Like I said earlier, I have always had the view of “let’s leave things as natural as possible and only intervene when necessary.” After listening to many, many podcast episodes and reading many many stories, I realized that MANY women have had similar experiences. I was not the only woman who felt like birth was done to me, rather than being a mother who gave birth. Yes, I’m alive. Yes, my baby is alive. But I think I should feel like more than just a body on the table (or bed) that they’re trying to get a baby out of as fast as possible. We are the mothers. We grow these babies. We deliver them, be it vaginally or straight out of the abdomen. Then we nurture them and introduce them to this big world. We’re the only home they know. We’re not just a body on the table. We matter. Both our physical and mental well-being are important.
It got me thinking about my first two birth stories.
Part of me wonders if all three of my births are connected. With our first baby, they kept ramping up the Pitocin to “help things progress” more quickly. As a result, I went from dilated to 6cm to him in my arms within two hours. They had to triple the post-delivery Pitocin dosage, gave me an emergency clotting shot in my thigh, and a rectal pill to slow the bleeding. Meanwhile, the doctor had to repeatedly reach in and pull clots out as my uterus contracted back down and nurses performed a lot of fundal massage (yes, that was all still completely unmedicated). Looking back on it after Arlo’s birth, it felt like my first birth was done to me also. Did the Pitocin push my body too hard and fast cause the hemorrhage? Did all the pulling and manual sweeping of blood clots cause some scarring? If there was some scarring, did that cause the issues with our second baby implanting correctly, which caused all her issues? I don’t know. I’ve never gone through labor and delivery without Pitocin.
With our second baby, we induced her due to the complications I talked about earlier – Pitocin again. Once she was safely delivered, the doctor proceeded with the standard procedure to gently pull on the umbilical cord while the nurse applied counter pressure to my uterus to help deliver the placenta. I ended up with a piece of retained placenta that I had to go back in for the D&C to remove a few weeks later. Did the cord traction cause the placenta to break away before it was quite ready and leave a piece behind? Would the placenta have ever released on its own? It can be a cause of hemorrhage, which is why they try to apply traction to release it sooner rather than later. But did it cause more scarring? Did the D&C cause some unknown abnormalities?
Was Arlo breech because I had some scarring in my uterus and it wasn’t quite the right shape?
I don’t know.
I won’t ever know.
But as I started to work through everything that happened with Arlo, I felt like I also had to work through reverse trauma from my first two babies.
On the one hand, I was young and naïve when I went in to deliver my first baby. So I just trusted what the doctors were doing. I wish they had sent me home and told me to come back when I was really in active labor, rather than admit me and crank the Pitocin. Why do they do that? Why not leave my body alone and let it do what it needs to do on its own? My water wasn’t broken and I was still one day before the due date. Why was that the standard procedure? Birth shouldn’t have to be medicalized all the time.
On the other hand, I feel that western medicine saved our second baby’s life. There were some major issues during her pregnancy and I truly feel that she would not have survived had I carried her to term. I just knew that she needed to be induced and born. When she was born, the placenta was completely gray, flat, and the cord had attached to the thinnest side (since it was flat, rather than nice and round). The placenta was almost completely dead. After seeing the condition of it, I don’t know if she would have made it one more day, let alone to her due date. That beautiful mom-baby connection again.
But how do I reconcile all these different experiences?
I don’t know.
But I’m a thinker and process everything, including trauma, by reading and learning and finding some sort of understanding of how, or why, things end up they way they do.
I have had a hard time putting words to my thoughts on the whole issue of western medicine versus holistic medicine. But I saw an Instagram post the other day that perfectly summed it up. This is what she said:
“In the past week, I’ve drunk raw milk from our family cow and birthed our seventh baby at home with no medications. I also had one of our kids undergo surgery and gave antibiotics and other drugs to our beloved cow. It is all about balance and making informed decisions for your family. Accept that our world is broken and there is no perfect answer.” From @bethdeclercq.
I guess I’m still processing and learning from Arlo’s birth because it brought tears to my eyes when I read it. It’s so true. There is a time and place for both natural medicine and western medicine. There’s a reason we have present-day medicine. There’s a reason we’ve had natural medicine for thousands of years. Both have value. Both are good. Both are necessary.
Our world is broken and there is no perfect answer.
A Lesson from Grandma
A few weeks after Arlo’s birth, I watched my grandma pass away. I had never seen anyone die. Next to birth, it was the most beautiful thing I’ve ever witnessed – new life and the end of this life, how ironic.
During the weeks leading up to the c-section, I was so afraid of hemorrhaging if I ended up in c-section. I was afraid of what that might mean in addition to my anemia. I’ll be honest, I was afraid I might die, or our baby might die. I just felt very close to death at a time when I wanted to feel very close to new life. And in the moment that I watched my grandma pass away, it hit me. We all end up right there. That’s it. This is the only life we have. Right now. Today. No one knows what tomorrow brings or when our time will be up. We all end up at the same spot. We will all end up right there.
The combination of feeling very close to death and then watching my grandma pass through it was one of the most powerful lessons in my entire life. A year and a half later, and those few weeks around his birth and the death of my grandma are the most pivotal of my entire life. It changed my perspective forever. Who do I want around me when I lay on that death bed? What do I want to say I did with my life? Where are my priorities?
Lean In
I decided to lean in. To lean in to others in their brokenness. To lean into my own hurt. To lean in to life.
I had always talked about running a half marathon. But it was more of an “oh yeah, that would be cool to do someday.” I wasn’t sure I’d ever have the gumption to actually do it. No more. Just shy of one year after that c-section and I finished my first half marathon. And, funny coincidence, all those hours of running? Yes, they helped heal me physically, but, more than anything, mentally. Something about facing a challenge that I actually had control over. I have never been a long distance runner. I always said I could never be a long distance runner. I always told myself I just wasn’t built for it. Nope. No more. We only get one life.
I started to take a more proactive approach to mine and our family’s health. We have always been active, generally healthy, and exercised regularly. But I poured myself into researching more whole-person health & wellness. I spurred a big shift in how I now approach health & wellness for our entire family. I’ll never have all the answers for why my births have gone the ways they did, but I now have a lot more knowledge of the things I do have control over that affect our healthy & wellness. And I can take action on those things – creating a more toxin free home, daily exercise, the food we eat, etc.
Those few weeks also promted the entire rebrand of this small business of mine. I realized I wanted to slow down, focus on being a better mom and homemaker, not be stressed about trying to fit in my woodworking and massive renovations all the time. Don’t get me wrong, I love building and renovating. Always have. Always will. But I had talked about slowing down for so long, especially in this phase of life with little kids. I don’t want to miss it. And I finally realized it’s now or never. No time like the present. Who knows what tomorrow will bring.
I want to live every day on purpose.
I am going to live every day on purpose.
On Purpose
My husband Joseph is wise beyond his years. I could not have gotten through any of this without him, and one of the most noteworthy things he kept repeating to me was this:
None of us gets to choose the trials we’re handed in life. The only thing we have control over is how to respond to it.
Powerful.
With each challenge or trial we face, it really boils down to two options – to learn and grow from it, or to become bitter and angry.
Yes, Arlo’s birth was traumatic. But I am now at a place that I am so thankful it happened. I see God’s hand in all of it.
Thank God for a traumatic birth so I could learn to be there for others in their trials.
Thank God for a birth that opened my mind to learn about different approaches to health & wellness so I can build and nurture a healthy home for our family.
Thank God for my grandma, who’s beautiful passage from this life pushed me in the right direction – to learn and grow from a difficult time.
Thank God for a husband full of patience and wisdom.
Without any of these things, I never would have become the person I am today.
If you’ve had a traumatic birth and you’re not there yet, that’s ok. It is ok to say it was traumatic. It is ok to mourn your birth. It is ok to be thankful and hurt at the same time. Just start there.
Give yourself time. Be patient with yourself. Let yourself work through it. Tell the story (it helps a lot).
And then lean in.
You will feel like yourself again. There is beauty in this.

| Tylynn |
